Yeast infections are a common type of fungal infection that can affect different parts of the body, including the vagina, skin, mouth, and even the penis.
They are usually caused by an overgrowth of a fungus called Candida, which naturally lives in the body but can multiply when the balance of bacteria and yeast is disrupted.
Many people search online to understand what a yeast infection looks like, especially when they notice unusual symptoms such as itching, redness, rash, or unusual discharge.
The appearance of a yeast infection can vary depending on where it occurs. For example, a vaginal yeast infection may cause thick white discharge and swelling, while a skin yeast infection often appears as a red, itchy rash.
Oral yeast infections, also known as thrush, can produce white patches inside the mouth. Recognizing the signs of yeast infection early can help people seek proper treatment and prevent symptoms from becoming more uncomfortable or severe.
What Is a Yeast Infection?
A yeast infection is a fungal infection caused by an overgrowth of a type of yeast called Candida. This fungus naturally lives in small amounts on the skin, in the mouth, and in areas such as the digestive and genital tracts. Under normal conditions, beneficial bacteria and the body’s immune system keep the growth of Candida under control. However, when this balance is disrupted, the yeast can multiply rapidly and lead to an infection.
Yeast infections can affect several parts of the body. The most common type is a vaginal yeast infection, which affects many women at least once in their lifetime. However, yeast infections can also occur on the skin, in the mouth (a condition called oral thrush), and even on the penis in men. These infections often develop in warm, moist areas of the body where yeast can easily grow.
Several factors can increase the risk of developing a yeast infection. Taking antibiotics is one of the most common causes because antibiotics can kill the healthy bacteria that normally keep yeast levels balanced. Hormonal changes during pregnancy or from birth control pills may also trigger yeast overgrowth. Other risk factors include diabetes, a weakened immune system, tight clothing that traps moisture, and high sugar levels in the body.
Although yeast infections are usually not serious, they can cause uncomfortable symptoms such as itching, irritation, redness, and unusual discharge. Understanding what causes a yeast infection and how it develops is an important step toward recognizing its symptoms and finding the right treatment.
What Does a Yeast Infection Look Like?
The appearance of a yeast infection can vary depending on where it develops, but there are several common visual signs that help identify it. In many cases, a yeast infection causes noticeable redness, irritation, and swelling in the affected area. The skin may appear inflamed and sensitive, often accompanied by intense itching or a burning sensation. These symptoms can make the area feel uncomfortable, especially during movement or contact.
One of the most recognizable signs of a yeast infection is the presence of a rash. This rash is often bright red and may have slightly raised edges. In skin yeast infections, the rash can sometimes include small red bumps or spots around the main irritated area. These smaller bumps are often referred to as “satellite lesions” and are a common indicator of fungal infections caused by Candida.
Texture changes in the skin are also common. The affected area may look shiny, moist, or slightly cracked. In some cases, the skin may become dry and flaky, especially if the infection has been present for several days. People may also notice peeling or scaling around the irritated skin.
Another important sign is discharge, particularly in vaginal yeast infections. The discharge is typically thick, white, and clumpy, often described as having a “cottage cheese” appearance. Unlike some other infections, yeast infections usually do not produce a strong odor.
What Does a Vaginal Yeast Infection Look Like?
A vaginal yeast infection is one of the most common types of fungal infections and is usually caused by an overgrowth of Candida. Many women experience this condition at least once in their lifetime. Understanding what a vaginal yeast infection looks like can help identify the problem early and seek proper treatment.
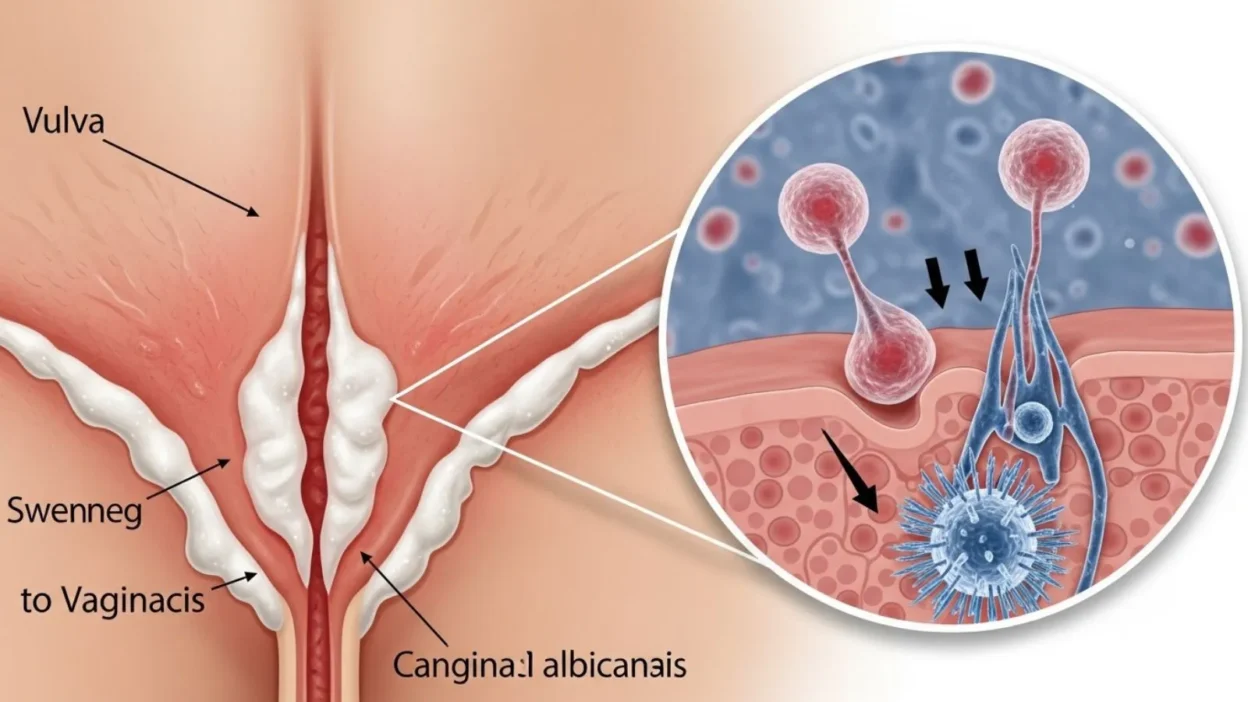
One of the most noticeable signs is thick white vaginal discharge. This discharge is often described as having a “cottage cheese” appearance because it looks clumpy and dense. Unlike some other vaginal infections, the discharge from a yeast infection usually does not have a strong or unpleasant odor. However, the amount of discharge may increase and cause discomfort throughout the day.
The vulva, which is the outer part of the female genital area, may also show visible changes. The skin around this area often becomes red, swollen, and irritated. In some cases, the skin may appear shiny or slightly inflamed. Severe irritation can sometimes lead to small cracks or soreness in the skin, especially if the itching is intense.
Another common symptom is persistent itching and burning around the vaginal opening. This itching can become worse at night or after physical activity. Some women may also experience burning during urination or pain during sexual intercourse, which can make daily activities uncomfortable.
What Does a Male Yeast Infection Look Like?
Although yeast infections are more commonly associated with women, men can also develop them. A male yeast infection is usually caused by the same fungus, Candida, and often affects the head of the penis. This condition is sometimes referred to as candida balanitis. Understanding what a male yeast infection looks like can help men recognize symptoms early and seek proper treatment.
One of the most common visible signs is a red rash on the head of the penis. The skin may appear inflamed, irritated, and slightly swollen. In some cases, the affected area may look shiny or moist. Small red spots or patches may also develop, making the irritation more noticeable.
Another symptom that may appear is white patches or a thick, white substance on the skin of the penis. This can sometimes resemble the discharge seen in other types of yeast infections. The skin may also become dry, cracked, or flaky, especially if the infection has been present for some time.
Men with a yeast infection often experience itching, burning, or irritation around the affected area. The discomfort may become more noticeable after urination or sexual activity. In some cases, there may also be a mild unpleasant odor due to the buildup of yeast and moisture.
Risk factors for male yeast infections include poor hygiene, diabetes, a weakened immune system, or sexual contact with a partner who has a yeast infection. Identifying these signs early can help men begin treatment and prevent the infection from worsening.
What Does a Skin Yeast Infection Look Like?
Yeast infections aren’t limited to the genital area—they can also occur on the skin, particularly in warm, moist areas of the body. These skin yeast infections are commonly caused by an overgrowth of Candida and often appear in skin folds, such as under the breasts, armpits, groin, or between the toes. Understanding the visual signs can help identify and treat the infection promptly.
A key feature of a skin yeast infection is a red, inflamed rash. The affected skin may look bright red and feel warm to the touch. In many cases, the rash has slightly raised edges and may be surrounded by small satellite bumps or pustules, which are tiny red spots that often develop near the main rash. These “satellite lesions” are a hallmark of yeast-related skin infections.
The texture of the skin can also change. The area may appear shiny, moist, or even cracked in severe cases. In some instances, the skin may peel or flake, especially if the infection has persisted for several days. Itching and burning sensations are common, and scratching can further irritate the skin, sometimes leading to secondary bacterial infections.
Skin yeast infections are more likely to develop in individuals who sweat excessively, wear tight or non-breathable clothing, or have a weakened immune system. People with diabetes or obesity are also at higher risk.
Recognizing the appearance of a skin yeast infection is important because early treatment with antifungal creams or medications can prevent the infection from spreading and reduce discomfort. Keeping the affected area clean and dry is also essential for recovery.
What Does Oral Yeast Infection (Thrush) Look Like?
Oral yeast infections, commonly known as thrush, occur when the fungus Candida overgrows in the mouth or throat. This type of yeast infection can affect people of all ages, including infants, adults, and individuals with weakened immune systems. Recognizing what oral thrush looks like is important for early treatment and to prevent discomfort while eating or speaking.
The most noticeable sign of oral yeast infection is the presence of white patches or plaques inside the mouth. These patches often appear on the tongue, inner cheeks, roof of the mouth, and sometimes the gums or tonsils. They may look creamy or slightly raised, and trying to scrape them off can leave red, inflamed tissue underneath, which may bleed slightly.
Other visible signs include redness and swelling in the affected areas, making the mouth feel sore or tender. Some people experience a burning sensation or discomfort while eating, especially when consuming acidic or spicy foods. In severe cases, the infection can spread to the throat, causing difficulty swallowing.
Oral thrush can also affect infants, appearing as white patches on the tongue or inside the cheeks, which can make feeding uncomfortable. Adults with weakened immune systems, diabetes, or those using inhaled corticosteroids are also at higher risk.
Early recognition of thrush is crucial because antifungal treatments, such as oral lozenges or mouth rinses, are highly effective. Maintaining good oral hygiene, rinsing the mouth after using inhalers, and controlling blood sugar levels can help prevent recurrence. Understanding the visual and symptomatic signs of oral yeast infection helps in prompt diagnosis and reduces complications.
Yeast Infection vs Other Conditions
Not all rashes, irritation, or unusual discharge are caused by yeast infections. Many conditions share similar symptoms, making it important to differentiate a yeast infection from other health issues. Understanding these differences can prevent misdiagnosis and ensure proper treatment.
One common condition often confused with yeast infections is bacterial vaginosis (BV). BV typically causes a thin, grayish or yellowish vaginal discharge with a strong odor, unlike the thick, white “cottage cheese” discharge of a yeast infection. Redness and itching are usually less severe in BV, and it may require antibiotics rather than antifungal treatment.
Sexually transmitted infections (STIs) such as trichomoniasis, chlamydia, or gonorrhea can also produce discharge and irritation. STIs may cause pain during urination or sexual intercourse, unusual odor, and in some cases, sores or lesions, which are not typical of yeast infections.
Allergic reactions or contact dermatitis can cause rashes and itching in genital or skin areas, similar to yeast infections. However, allergic reactions usually appear shortly after exposure to a new soap, detergent, or fabric, and the skin may have a more widespread, patchy appearance rather than the localized redness and satellite lesions of a yeast infection.
Jock itch (tinea cruris) is another fungal infection that resembles a yeast infection but is caused by dermatophyte fungi. It typically affects men in the groin area, forming a ring-shaped, red rash with a clear edge, while yeast infections tend to produce satellite bumps and moist skin folds.
Careful observation of symptoms, appearance, and discharge type helps distinguish yeast infections from these other conditions. When uncertain, consulting a healthcare provider ensures an accurate diagnosis and effective treatment.
Causes of Yeast Infections
Yeast infections occur when there is an overgrowth of the fungus Candida, which normally lives in small amounts in the body. While Candida is usually harmless, certain factors can disrupt the natural balance of bacteria and yeast, allowing it to multiply and cause infection. Understanding these causes can help prevent and manage yeast infections effectively.
One of the most common triggers is the use of antibiotics. Antibiotics kill not only harmful bacteria but also the beneficial bacteria that keep yeast growth in check. This imbalance can lead to an overgrowth of Candida, especially in the vaginal area.
Hormonal changes also play a significant role. Women may experience yeast infections during pregnancy, while taking birth control pills, or during hormonal fluctuations related to the menstrual cycle. These changes can alter the vaginal environment, making it easier for yeast to thrive.
Individuals with high blood sugar or diabetes are at increased risk, as yeast feeds on sugar. Poorly controlled blood sugar levels create an ideal environment for yeast to grow, increasing the likelihood of infection.
A weakened immune system, whether due to illness, medications, or chronic conditions, can reduce the body’s ability to keep yeast growth under control. Similarly, tight or non-breathable clothing can trap moisture and heat, creating favorable conditions for skin yeast infections.
Other factors include excessive sweating, poor hygiene, stress, and a diet high in sugar or refined carbs. Recognizing these causes can help individuals take preventive steps, such as wearing breathable fabrics, managing blood sugar, and using antibiotics cautiously. Early awareness of risk factors reduces the chance of recurring yeast infections.
When Should You See a Doctor?
Most yeast infections are mild and can be treated with over-the-counter antifungal medications or home remedies. However, there are situations where medical evaluation is necessary to ensure proper treatment and rule out other conditions. Recognizing when to see a doctor is crucial for preventing complications and prolonged discomfort.
You should seek medical attention if your yeast infection symptoms are severe or persistent. Severe itching, burning, redness, or swelling that does not improve within a few days of treatment may indicate a more serious infection or a resistant strain of Candida. Similarly, if symptoms last longer than a week despite home treatment, a healthcare professional should evaluate you to confirm the diagnosis.
Recurring yeast infections are another reason to consult a doctor. Experiencing four or more yeast infections within a year may indicate an underlying health issue, such as diabetes, hormonal imbalance, or an immune system problem. Your doctor can perform tests to determine the cause and recommend a long-term treatment plan.
Medical attention is also recommended if you notice unusual symptoms such as fever, pain during urination, sores, or an unusual discharge that differs from typical yeast infection symptoms. These could indicate other infections, including sexually transmitted infections, which require different treatments.
Pregnant people, individuals with chronic illnesses, or people with weakened immune systems should seek guidance promptly if they suspect a yeast infection. Early medical intervention ensures safe and effective treatment, reduces discomfort, and prevents the infection from spreading to other parts of the body.
Treatment Options for Yeast Infections
Yeast infections are generally treatable with a combination of over-the-counter medications, prescription drugs, and home remedies, depending on the severity and location of the infection. Early treatment can relieve discomfort, prevent the infection from worsening, and reduce the risk of recurrence.
For most vaginal yeast infections, antifungal creams, ointments, or suppositories are commonly used. These treatments, such as clotrimazole or miconazole, are applied directly to the affected area and typically provide relief within a few days. Oral antifungal medications like fluconazole are also available for more severe or recurrent infections and are usually prescribed by a healthcare provider.
Male yeast infections can be treated with topical antifungal creams applied to the affected area. Keeping the skin clean and dry during treatment is essential for faster recovery. Similarly, skin yeast infections in areas like skin folds respond well to antifungal creams or powders, which help reduce moisture and control fungal growth.
Oral yeast infections (thrush) require antifungal solutions, lozenges, or gels that are applied inside the mouth. These treatments help eliminate the white patches, relieve pain, and prevent the infection from spreading to the throat or digestive system.
In addition to medications, home care can support recovery. This includes wearing breathable clothing, keeping affected areas dry, practicing good hygiene, and avoiding irritants such as scented soaps or tight clothing. Reducing sugar intake may also help prevent future infections, as yeast thrives on sugar.
How to Prevent Yeast Infections
Preventing yeast infections involves maintaining a healthy balance of bacteria and yeast in the body and reducing factors that encourage fungal overgrowth. Simple lifestyle changes and hygiene practices can significantly reduce the likelihood of developing an infection.
One of the most effective preventive measures is keeping the affected areas clean and dry. Yeast thrives in warm, moist environments, so it’s important to thoroughly dry skin folds, the genital area, and other susceptible regions after bathing or sweating. Using breathable clothing made of cotton or moisture-wicking fabrics can also reduce moisture buildup and limit fungal growth.
Maintaining good personal hygiene is essential. This includes regular bathing, changing underwear daily, and avoiding harsh soaps, scented washes, or perfumed wipes that can disrupt the natural balance of bacteria and yeast. For women, wiping from front to back after using the bathroom helps prevent yeast from spreading.
Diet and lifestyle factors also play a role in prevention. Limiting sugar and refined carbohydrates can help reduce yeast overgrowth, as yeast feeds on sugar. Managing chronic conditions such as diabetes and supporting the immune system through proper nutrition, sleep, and stress management are also important.
Women using antibiotics or hormonal medications should be aware that these can increase the risk of yeast infections. In such cases, discussing preventive measures with a healthcare provider may be beneficial.
By combining hygiene, clothing choices, diet, and lifestyle habits, it’s possible to lower the risk of yeast infections significantly. Early attention to symptoms and preventive practices helps maintain comfort and overall health.
Frequently Asked Questions (FAQs) About Yeast Infections
1. What color is yeast infection discharge?
In vaginal yeast infections, the discharge is typically thick, white, and clumpy, often described as “cottage cheese” in texture. Unlike bacterial infections, it usually does not have a strong odor.
2. Do yeast infections cause a smell?
Most yeast infections have little to no odor. If there is a noticeable smell, it may indicate another type of infection, such as bacterial vaginosis or a mixed infection, which requires medical evaluation.
3. Can men get yeast infections?
Yes, men can develop yeast infections, often appearing as red, itchy rashes or white patches on the penis. Risk factors include poor hygiene, diabetes, sexual contact with an infected partner, or a weakened immune system.
4. How long does a yeast infection last?
With proper treatment, most yeast infections resolve within 3 to 7 days. Severe or recurrent infections may take longer and require prescription medication.
5. Can yeast infections go away on their own?
Mild yeast infections may sometimes improve without treatment, but self-resolution is not guaranteed, and symptoms can worsen or recur. Using antifungal medications ensures faster relief and reduces complications.
6. Are yeast infections contagious?
While not classified as a sexually transmitted infection, yeast infections can be passed between sexual partners, especially if one partner has active symptoms.
7. How can I prevent yeast infections?
Prevention involves keeping affected areas dry, practicing good hygiene, wearing breathable clothing, reducing sugar intake, and managing risk factors like diabetes or frequent antibiotic use.
Conclusion:
Yeast infections are a common fungal condition that can affect different parts of the body, including the vagina, skin, mouth, and penis.
Recognizing what a yeast infection looks like such as redness, itching, rashes, thick white discharge, or oral patches is essential for early identification and effective treatment.
Different types of yeast infections have unique visual signs, but all share a common factor: Candida overgrowth. Understanding the causes, risk factors, and preventive measures can help reduce the likelihood of infections.
Maintaining proper hygiene, wearing breathable clothing, managing blood sugar, and using medications carefully are all key steps in prevention.
While most yeast infections respond well to over the counter or prescription antifungal treatments, it’s important to consult a doctor for severe, persistent, or recurring cases. Early recognition and proper care ensure quick relief, prevent complications, and support long-term health.

The author behind RiddleBurst.com loves creating fun, clever, and unique riddles for all ages. Their goal is to challenge minds, bring smiles, and make learning through riddles both engaging and enjoyable.