Sciatica is a common condition that affects millions of people worldwide, yet many struggle to describe exactly what it feels like.
Unlike general back pain, sciatica stems from irritation or compression of the sciatic nerve, which runs from the lower back down through the legs.
The sensations can vary widely, from sharp, shooting pain and burning discomfort to tingling, numbness, or weakness in one leg.
Because the pain can mimic other conditions, it’s often confusing to identify at first.
Understanding what sciatica feels like is crucial for recognizing the condition early and seeking effective relief.
In this article, we’ll break down the different types of sciatica pain, where it occurs, how it impacts daily activities, and when to consult a healthcare professional.
If you’re experiencing mild discomfort or severe nerve pain, this guide will help you understand your symptoms and take steps toward relief.
What Is Sciatica?
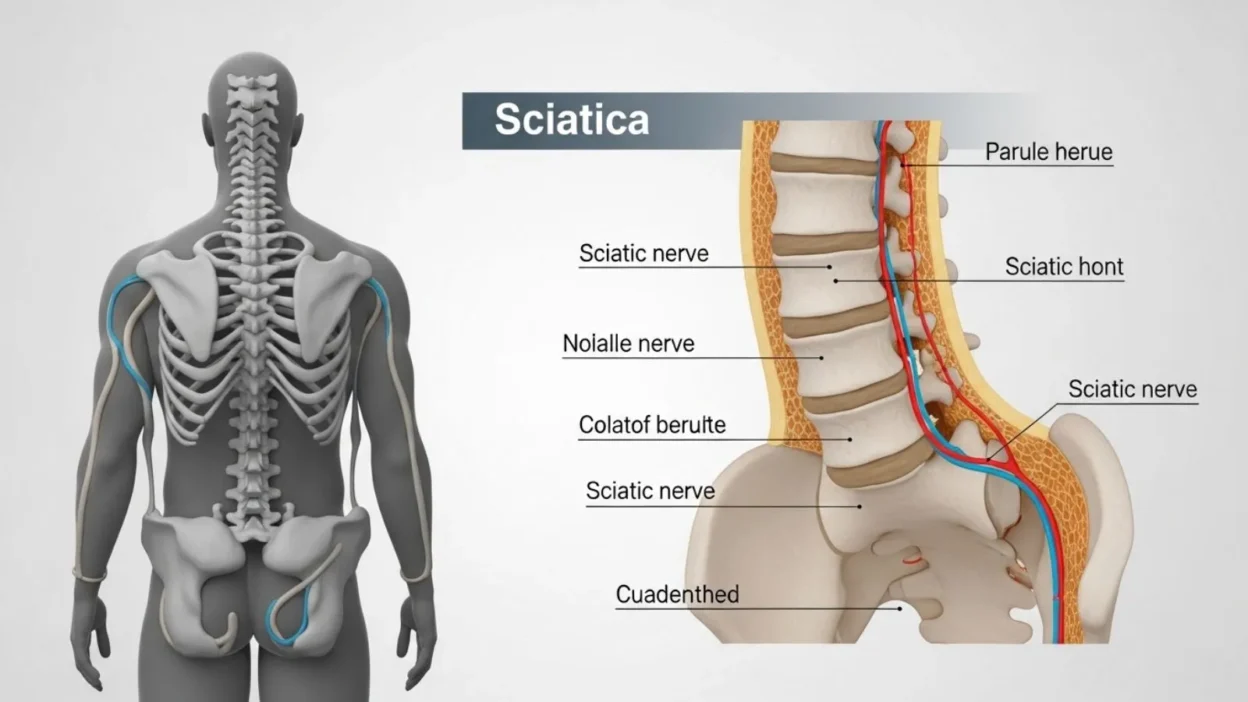
Sciatica is not a disease itself but a symptom of an underlying issue involving the sciatic nerve, the longest nerve in the body. It originates in the lower back, travels through the hips and buttocks, and extends down each leg. When this nerve becomes compressed, irritated, or inflamed, it can trigger the distinctive pain known as sciatica.
The most common causes include a herniated or bulging disc, which puts pressure on the nerve roots, spinal stenosis (narrowing of the spinal canal), or piriformis syndrome, where the small piriformis muscle in the buttocks irritates the sciatic nerve. Less commonly, injuries, tumors, or infections in the spine can also cause sciatic pain.
Unlike general back pain that is usually localized, sciatica pain radiates along the path of the nerve, often affecting only one side of the body. People may experience discomfort in the lower back, buttocks, thigh, calf, or foot. The pain can vary in intensity from a mild, dull ache to sharp, burning, or shooting sensations.
Understanding the root cause is essential for proper treatment. While mild sciatica may improve with home care and lifestyle changes, persistent or severe symptoms require medical evaluation. Early recognition and intervention can prevent complications, reduce pain, and improve mobility, making it easier to manage this often-debilitating condition.
Common Sensations of Sciatica
Sciatica can feel very different from person to person, which is why it’s often confusing to identify at first. The sciatic nerve carries signals from the lower back to the legs, so irritation along this pathway can produce a variety of sensations. One of the most common symptoms is sharp, shooting pain that travels from the lower back or buttocks down the leg. Many people describe this as a sudden jolt or electric-like shock that can make standing or walking difficult.
Another frequent symptom is burning or tingling, sometimes described as “pins and needles.” This sensation can extend from the buttocks to the calves and feet, and may feel worse when sitting for long periods or standing up suddenly. Numbness or weakness in the leg is also common, making it hard to move the foot or lift the leg comfortably. Some individuals notice that one leg feels heavier or weaker than the other.
The intensity of sciatica pain can vary widely. For some, it’s a mild discomfort that comes and goes, while for others, it’s a constant, intense pain that interferes with daily activities. Symptoms often worsen after long periods of sitting, sneezing, coughing, or lifting heavy objects. Understanding these common sensations can help distinguish sciatica from general back or leg pain and guide timely management and treatment.
Where Sciatica Pain Occurs
Sciatica pain typically follows the path of the sciatic nerve, which extends from the lower back, through the hips and buttocks, and down each leg. While the exact location can vary, most people experience pain on one side of the body rather than both. Understanding where sciatica commonly occurs can help distinguish it from general back pain or other conditions.
The most frequent starting point is the lower back, where nerve roots in the lumbar spine may be compressed or irritated. From there, pain often radiates through the buttocks, sometimes described as a deep, aching discomfort. Many individuals feel sharp or burning pain along the back of the thigh, which may extend to the calf and foot. Some even report tingling or numbness in the toes or soles, reflecting nerve involvement further down the leg.
Sciatica symptoms are often position-dependent. Sitting for long periods can intensify the pain in the buttocks and legs, while standing or walking may trigger shooting or electric-like sensations. Activities like bending, lifting, or twisting can also worsen the discomfort. For some, even a mild cough or sneeze can create sudden jolts of pain along the nerve pathway.
Visualizing the pain path can help patients identify sciatica early. Knowing that pain can travel from the lower back to the foot and may include tingling, numbness, or weakness can assist in distinguishing sciatica from muscular or joint-related issues, making timely intervention and relief more achievable.
How Sciatica Feels During Daily Activities
Sciatica can significantly affect everyday life, and its symptoms often become more noticeable during routine activities. Sitting for long periods, for example, can intensify discomfort, especially if the chair does not provide proper lumbar support. Many people report sharp, shooting pain in the buttocks or legs after extended sitting, sometimes making it difficult to stand up or shift positions comfortably.
Walking or standing can also trigger sciatica sensations. Some individuals experience burning or tingling that travels down the leg with each step, while others notice sudden jolts of pain when changing posture. These sensations can limit mobility and make simple tasks like climbing stairs, grocery shopping, or walking short distances challenging.
Sleeping may also be disrupted by sciatica. Lying in one position for too long can cause numbness or tingling, forcing frequent adjustments during the night. Certain sleeping positions, such as lying on the stomach, may worsen nerve irritation, while others, like lying on the back with a pillow under the knees, can help reduce discomfort.
Even everyday movements such as bending, lifting, or twisting can exacerbate sciatica pain. Sneezing or coughing may send sharp jolts down the leg due to increased pressure on the sciatic nerve. Recognizing how sciatica affects daily activities is essential for managing symptoms effectively. Simple adjustments in posture, movement, and ergonomics can help minimize discomfort and prevent flare-ups, allowing individuals to maintain more normal daily routines.
Sciatica vs. Other Types of Pain
Sciatica is often confused with general back or leg pain, but understanding the differences is key to proper diagnosis and treatment. Unlike typical muscle strain or lower back pain, which tends to be localized and dull, sciatica originates from irritation of the sciatic nerve and usually follows a specific pathway. Pain often radiates from the lower back or buttocks down the leg, sometimes reaching the calf or foot, whereas muscular pain rarely travels this far.
Muscle pain usually feels sore, stiff, or tight and improves with rest, stretching, or massage. In contrast, sciatic nerve pain can be sharp, burning, tingling, or electric-like, and may worsen with prolonged sitting, standing, or sudden movements like coughing or sneezing. Another distinction is numbness or weakness; sciatica can cause one leg to feel heavier or less responsive, a symptom rarely seen in simple back strain.
Hip or knee pain may also be mistaken for sciatica, but these issues generally do not involve tingling, numbness, or radiating leg pain. Understanding these differences is crucial for avoiding misdiagnosis and ensuring the correct treatment approach.
Recognizing whether the pain originates from nerve compression or a muscle/joint issue can help guide effective relief strategies. While home remedies may relieve mild muscular discomfort, persistent sciatica often requires targeted interventions like stretches, posture correction, physical therapy, or medical evaluation to prevent worsening nerve irritation.
Red Flag Symptoms: When to See a Doctor
While many cases of sciatica can be managed at home with stretches, posture adjustments, and over-the-counter pain relief, certain symptoms require immediate medical attention. Recognizing red flag signs can prevent permanent nerve damage and complications.
One of the most serious warning signs is severe leg weakness or foot drop, where lifting the foot becomes difficult or impossible. This indicates significant nerve compression and requires prompt evaluation. Another critical symptom is loss of bladder or bowel control, which may suggest cauda equina syndrome—a rare but urgent condition that needs immediate medical care.
Persistent or worsening pain that does not improve with home care is another reason to consult a doctor. Sciatica that interferes with daily activities, sleep, or walking for more than a few weeks should be evaluated to rule out underlying spinal conditions. Sudden, intense pain after an injury or accident also warrants medical attention.
Additional red flags include numbness spreading to multiple areas, severe radiating pain down both legs, or symptoms accompanied by fever, unexplained weight loss, or trauma. These signs may indicate more serious issues like infections, tumors, or severe disc herniation.
Early recognition and intervention can prevent long-term complications and improve recovery. If any of these symptoms occur, it’s important to seek prompt medical care, as timely diagnosis allows for targeted treatment—whether through physical therapy, medication, or surgical options—ensuring the best possible outcome for nerve health and mobility.
Relief and Management Options
Managing sciatica effectively requires a combination of home remedies, lifestyle adjustments, and medical interventions, depending on the severity of the symptoms. For mild to moderate sciatica, home treatments can provide significant relief. Applying ice or heat therapy to the lower back and buttocks can reduce inflammation and soothe nerve irritation. Alternating between cold and warm compresses may be especially effective during flare-ups.
Gentle stretching and exercises that target the lower back, hamstrings, and hips can help relieve pressure on the sciatic nerve. Movements like knee-to-chest stretches, piriformis stretches, and pelvic tilts are commonly recommended to improve flexibility and reduce pain. Maintaining proper posture while sitting, standing, or lifting is equally important to minimize nerve compression.
Over-the-counter medications, such as NSAIDs (ibuprofen, naproxen), can reduce inflammation and alleviate pain temporarily. However, prolonged use should be monitored by a healthcare professional. For more persistent or severe cases, physical therapy may be prescribed to strengthen the core, improve posture, and stabilize the spine, providing long-term relief.
In rare cases where conservative measures fail, medical interventions like steroid injections or surgery may be considered to relieve nerve pressure. It is crucial to consult a doctor before pursuing these options.
Combining these strategies with lifestyle changes—like regular movement, ergonomic adjustments, and weight management—can help manage sciatica effectively. Early and consistent management improves mobility, reduces discomfort, and prevents future flare-ups, allowing individuals to maintain a more active and pain-free life.
Prevention and Lifestyle Tips
Preventing sciatica or reducing the risk of flare-ups involves adopting healthy habits and lifestyle changes that protect the sciatic nerve and the lower back. One of the most important strategies is maintaining proper posture. Whether sitting, standing, or lifting, keeping the spine aligned reduces unnecessary pressure on the lower back and nerve roots. Ergonomic chairs, lumbar support cushions, and standing desks can make a significant difference for those who sit for long periods.
Regular exercise is another key factor. Strengthening the core, back, and leg muscles helps stabilize the spine and supports the sciatic nerve. Activities such as walking, swimming, yoga, or Pilates improve flexibility and reduce stiffness that can trigger sciatica. Stretching exercises targeting the hamstrings, hips, and lower back can further relieve tension along the nerve pathway.
Maintaining a healthy weight also plays a role in preventing nerve compression. Excess weight, especially around the abdomen, can increase stress on the lumbar spine, making sciatic symptoms more likely. Incorporating a balanced diet rich in anti-inflammatory foods can support overall spinal health.
Lifestyle adjustments, like avoiding prolonged sitting, taking regular movement breaks, and using safe lifting techniques, can prevent irritation of the sciatic nerve. Additionally, stress management and adequate sleep contribute to muscle relaxation and reduce chronic tension in the back.
By combining posture awareness, regular exercise, weight management, and mindful daily habits, individuals can reduce the frequency and intensity of sciatica pain, improve overall mobility, and support long-term nerve and spinal health. Prevention is always more effective than treating flare-ups after they occur.
FAQs About Sciatica
1. Does sciatica always cause back pain?
Not always. While many people experience lower back discomfort, sciatica primarily affects the sciatic nerve, so pain can also radiate through the buttocks, thigh, calf, and foot. Some individuals may feel leg pain without significant back pain.
2. How long does sciatica pain last?
The duration varies depending on the cause and severity. Mild sciatica can improve within a few weeks with home care and lifestyle changes, while chronic cases may persist for months and require medical treatment.
3. Can sciatica go away on its own?
Yes, in many cases, sciatica improves without surgery. Conservative measures like stretching, proper posture, physical therapy, and pain management can help the nerve heal and reduce inflammation. However, persistent or worsening symptoms should be evaluated by a healthcare professional.
4. Is surgery always necessary for sciatica?
Surgery is rarely the first option. It is usually considered only when conservative treatments fail or if there are severe symptoms, such as significant leg weakness, foot drop, or loss of bladder/bowel control. Most people experience relief through non-invasive methods.
5. How can I prevent sciatica flare-ups?
Maintaining good posture, staying active, strengthening the core, avoiding prolonged sitting, and managing weight are effective ways to reduce the risk of sciatica. Regular stretching and mindful movement habits also support spinal and nerve health.
Conclusion:
Sciatica can be a confusing and sometimes debilitating condition, but understanding what it feels like is the first step toward effective management.
From sharp, shooting pain and burning sensations to tingling, numbness, and leg weakness, the symptoms can vary widely, often affecting one side of the body. Recognizing the differences between sciatica and general back or muscle pain is essential for timely intervention.
While mild cases may improve with home care, stretching, and posture adjustments, persistent or severe symptoms require medical evaluation. Early recognition of red flag signs such as foot drop, loss of bladder or bowel control, or severe leg weakness can prevent complications and improve outcomes.
By combining proper treatment, daily lifestyle adjustments, and preventive habits like regular exercise, maintaining good posture, and managing weight, individuals can significantly reduce sciatica pain, improve mobility, and support long-term nerve health. Understanding your symptoms empowers you to take control and find relief, helping you stay active and pain-free.